Surgical Treatments for OSA
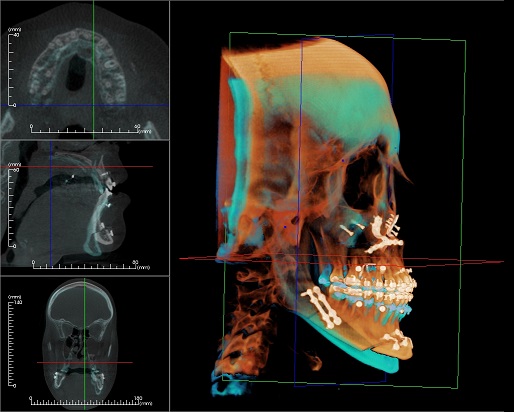
There are a variety of surgical treatments for Obstructive Sleep Apnea, targeting different anatomical problems. Surgery is often promoted as a one-time procedure that can correct the problem permanently. However, compared to CPAP and Oral Appliance Therapy, surgery is generally much less effective and the outcome less predictable. It’s difficult to generalize all surgical techniques given the variety of problems and corrective procedures, but the medical literature indicates that surgery is a less predictable option. Moreover, surgical operations depend on proper patient selection, patient-specific diagnostics, patient health and recoverability, individual doctors’ surgical skills, and a variety of other factors.
Surgical procedures have been developed for the various anatomical conditions affecting the airway. For patients considering surgery, it is important to receive a thorough evaluation and diagnosis to assess the specific anatomical cause of their Obstructive Sleep Apnea.
The following is a short review of some common surgeries, based on the anatomical areas that they target:
Nasal obstructions: Surgeries such as septoplasty and turbinate reduction are performed to correct nasal obstructions. These procedures alone may not always correct the problem and are often used in conjunction with CPAP or Oral Appliance Therapy given that the source of obstructions is often lower in the airway at the level of the soft palate and tongue. It is possible to have completely clear nasal passageways and still suffer from Obstructive Sleep Apnea. However, due to the importance of nasal breathing, these nasal surgeries may be recommended as adjunctive components of a complete treatment plan. Allergy and food sensitivity testing are also highly recommended for patients experiencing nasal congestion.
Reducing soft issues of the throat: There are multiple surgical techniques designed to reduce the soft issues of the throat, such as the soft palate, uvula, and pharyngeal tissues. A common and vey invasive one is called Uvulopalatopharyngoplasty (UPPP). UPPP has a relatively low success rate by itself, many potential complications, and a very difficult recovery. Recent modifications of this technique make it less invasive and more effective, however UPPP is still significantly less effective than non-surgical treatments such as CPAP and Oral Appliance Therapy. This is often the case because of the significant role of the tongue in Obstructive Sleep Apnea. The back of the tongue can easily block the airway when it falls backward during sleep.
Removing swollen adenoids and tonsils: Other soft-tissue surgeries focus on removing swollen adenoids and tonsils when they are diagnosed as the primary source of obstruction. These surgeries are usually successful and are recommended nearly universally when needed. It’s important to consult with an allergist and attempt to eliminate any allergies first before considering surgical approaches. Many patients are allergic to common elements in their environments or diets, which can easily be overlooked.
Snoring and breathing issues based on swollen adenoids and tonsils are most common in children, and it’s important to seek treatment in a timely manner so that their overall growth and development does not suffer. It is also important to consult with an airway-focused orthodontist as they can help grow and develop the orofacial-airway-related anatomy and thus the actual airway. It is recommended that children visit an orthodontist much earlier than traditionally thought as most airway-related problems begin early, before adult teeth are even present. An orthodontist can also help with discovery and treatment recommendations involving Orofacial Myofunctional Disorders (such as mouth breathing and tongue thrust) that may negatively impact children's facial and dental function, growth, and development.
Dental-skeletal anatomical relationships: Other surgical options aim to correct dental-skeletal anatomical relationships. Two common techniques are surgically assisted rapid palatal expansion (SARPE) and maxillomandibular advancement (MMA). These surgeries create more room in the oral cavity, which helps prevent the tongue and other soft tissues from relaxing into the airway and collapsing it during sleep. These techniques both involve skeletal surgery and the subsequent repostining of orofacial bones and teeth. They are usually much more successful and predictable treatments compared to other surgical techniques. However, they are very invasive, with long recovery times, and they must be combined with orthodontics to reposition the teeth into proper occlusion and esthetics. The cost, time, and surgical intensity are simply too much for many patients.
Patients considering in any surgical treatment for Obstructive Sleep apnea should weigh their options carefully and seek multiple opinions. Along with standard sleep studies, both proper diagnostics with proper diagnostic imaging techniques are essential before embarking upon any surgery. The selection of any surgical procedure is highly patient-specific, and there is no cure-all technique that applies to everyone.
It is important to note that surgical procedures alone are often not intended as the sole solution to OSA and are often used in combination with CPAP or Oral Appliance Therapy. A common example is turbinate reduction to help with nasal breathing in combination with Oral Appliance Therapy. This approach is called “Combination Therapy.” As a general rule, less invasive approaches should be tried first. If you have Obstructive Sleep Apnea and are considering any surgical treatment, please contact us if you have questions or would like a consultation about Oral Appliance Therapy as an alternative treatment or as part of a Combination Therapy approach.